
Dr Julie Choisne
One step at a time
In New Zealand children with cerebral palsy are not physically assessed until age six, in part because they need to be able to keep very still while 40 markers are exactingly fitted to their legs, and then be able to follow precise instructions about where and how to move in a purpose-built facility.
SfTI’s Julie Choisne is working on an alternative system that’s quick, mobile, inexpensive, and easy to fit to a child of any age.
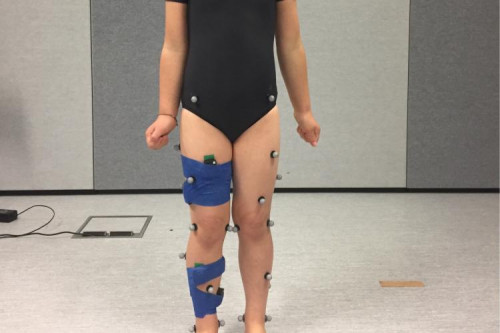
A research fellow at the University of Auckland, Julie has used SfTI Seed project funding to design sensors that are easy to strap onto a child’s ankles, knees and hips. The sensors collect information while the child walks or runs anywhere, including in the home or outside. With accompanying computer modelling, Julie can then analyse the way the child walks to learn what type of structural supports would be most helpful.
“It’s critical to understand how these children are moving as early as possible. If their foot, knee or hip isn’t moving normally, the child will develop a different gait to compensate and avoid pain. But moving differently puts abnormal mechanical loads on the bones that they’re not designed for, and that in turn causes deformation to the bone and an uncomfortable gait. The problem will continue to get worse as the bones keep growing and changing,” Julie says.
“If we can analyse the exact range of motion of the child’s joints while they walk, clinicians can prescribe the right Ankle Foot Orthosis design that supports the bones into the correct alignment so they can grow in the right way without it being painful.”

She says catching things early can mean the difference between a child being able to walk almost normally, or not at all.
Currently New Zealand’s only gait assessment centre is in Auckland, and children and their families must travel there to get properly assessed. The $800,000 motion capture system requires the precision placement of 40 markers on the child’s legs and torso, taking about an hour to set up, followed by recording the child walking in a large, purpose-built, low-light facility. The data is then analysed, and the required orthosis is ordered from the United States, usually taking several weeks to arrive.

Julie says her system would be likely to cost around $10,000 a unit and could be fitted by anyone, including the child themselves. There are no special facilities required, beyond the strap-on sensors and an iPad.
“They can then go off and play and walk around, and the sensors will download the information wirelessly to the iPad. The computer modelling side of the research then interprets the gait.”
To date the sensors and modelling have proven very good at predicting the accuracy of knee joint movements – about 95 percent accuracy when compared with the traditional method of assessment. The hip joint has also been very good at about 80 percent accuracy.
“The ankle joints are more challenging as there’s a lot more noise in the sensor data, so there’s still some work to do on that part.”
Until now the computer modelling has been developed from measurements of adults, rescaled for children. Julie has recently been awarded a further grant from the Health Research Council of New Zealand to refine her modelling using machine learning based on children (aged four to 18) postmortem CT scans collected by the Victorian Institute of Forensic Medicine in Australia.
She will use this data to build personalised bone models of children to increase the accuracy of computational models of both normal and abnormal development.
Another focus for the future is the potential of using 3D printing to manufacture personalised orthoses.
“At the moment, the prescriptions for these are sent to the US, and can take weeks to return. Meanwhile, children’s bones are growing all the time, and it’s not long before adjustments are needed in response to that growth. We’d like to explore the possibility of cost-effective alternatives like 3D printing using carbon fibres that could be ready as soon as the next day.
“We are working hard to be able to bring the tech to local doctors’ offices, and we’re excited about the big differences we hope to make for these children, their families and the medical community.”
Cerebral palsy is the leading cause of childhood physical disability, affecting 17 million children worldwide and 12,000 in New Zealand.
The condition is caused by damage to the parts of the brain that control movement, balance, and posture.
Listen to Julie chat about her work on The University of Auckland's 95bfm
Top image: Research Fellow, Auckland Bioengineering Institute, The University of Auckland, Julie Choisne: Image courtesy The University of Auckland.